Conversely AI analyzes every health insurance conversation to deliver insights that increase conversions, reduce cost per acquisition, and result in compliant, high-LTV enrollments.
Real-Time Call Insights
Conversely AI analyzes 100% of health insurance conversations to deliver daily insights, benchmark agent performance, and surface targeted recommendations. From handling objections to identifying bad habits and conversion bottlenecks, teams gain clear guidance to improve enrollment outcomes across the organization.
The Result?

Effortless Sales QA & Compliance at Scale
Conversely AI analyzes 100% of health insurance calls to automate quality assurance and compliance monitoring.
Customized scorecards, automatic tagging of required disclosures, and audit-ready trails give teams visibility into agent behavior while reducing QA costs. This addresses issues before it impacts revenue or CMS outcomes.
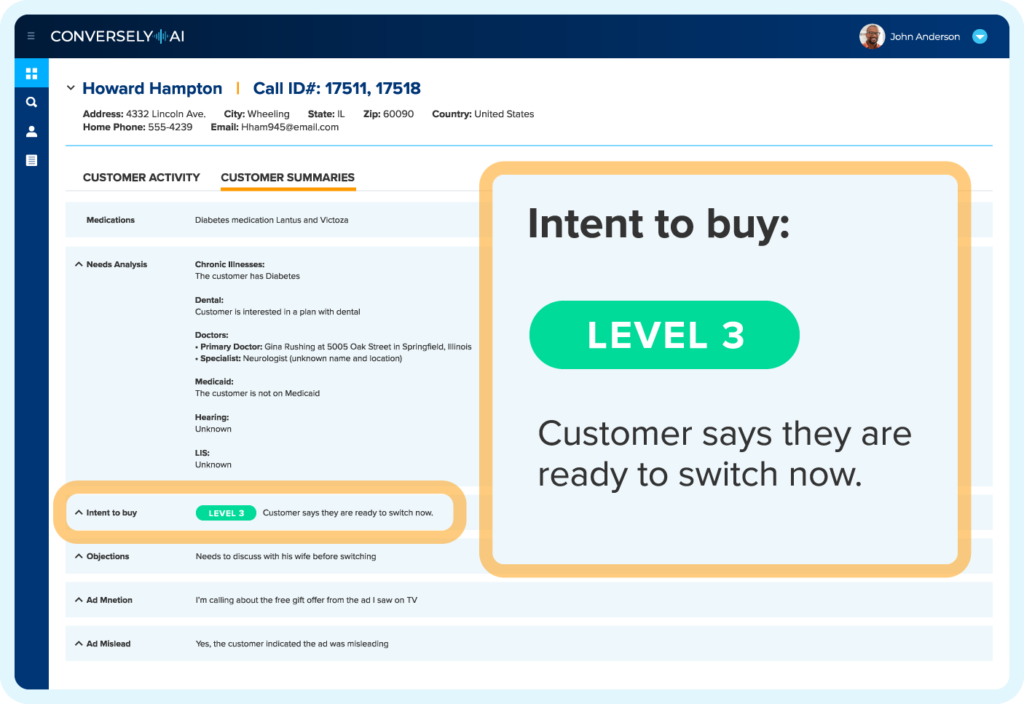
Know Your Leads Are Compliant & High Intent
Impact by Role
For Executives
Drive predictable growth, reduce compliance risk, and scale performance with full visibility across your sales operation.
Conversely AI tracks the full lifecycle of every lead, from initial contact to enrollment. Using AI-driven insights, it identifies underperforming leads, monitors agent follow-up, and highlights which affiliates generate the best ROI. This helps companies focus on high-quality leads and boost conversion rates while reducing wasted spend.
Yes.
Conversely AI links lead quality and agent performance back to your marketing campaigns. You can see which campaigns generate enrollable leads, which affiliates perform best, and which calls need improvement—helping your marketing team optimize targeting and reduce wasted spend.